Ultrasound of the Week #011
Case:
A 77 year old gentleman was admitted having had a fall and long lie, requiring the ambulance services to break into his home for access.
PMH : arthritis and depression, hadn’t seen a Doctor in 10 years.
After some time in department he was noted to be less responsive and was sent for CT. On route to CT he became pale, unresponsive and dropped his RR to 8. He was rushed to resus as he was peri-arrest and assessed there. He regained consciousness shortly after arrival in resus and his colour improved.
Examination: clear chest, cold to forearms peripherally, central CRT 3 seconds peripherally 5 seconds, ejection systolic murmur radiating to carotids. Neuro exam grossly normal.
POCUS revealed the following:
AAA: no abdominal aortic aneurysm noted
This was a difficult study due to very low body habitus and patient positioning. However, the following pertinent findings can be appreciated:

[expand title=”Interpretation:” tag=”h2″]
PLAX:
- The LV walls appear hypertrophied. The LV function appears grossly normal
- There is no pericardial/pleural effusion
- The AV appears heavily calcified and is hardly moving

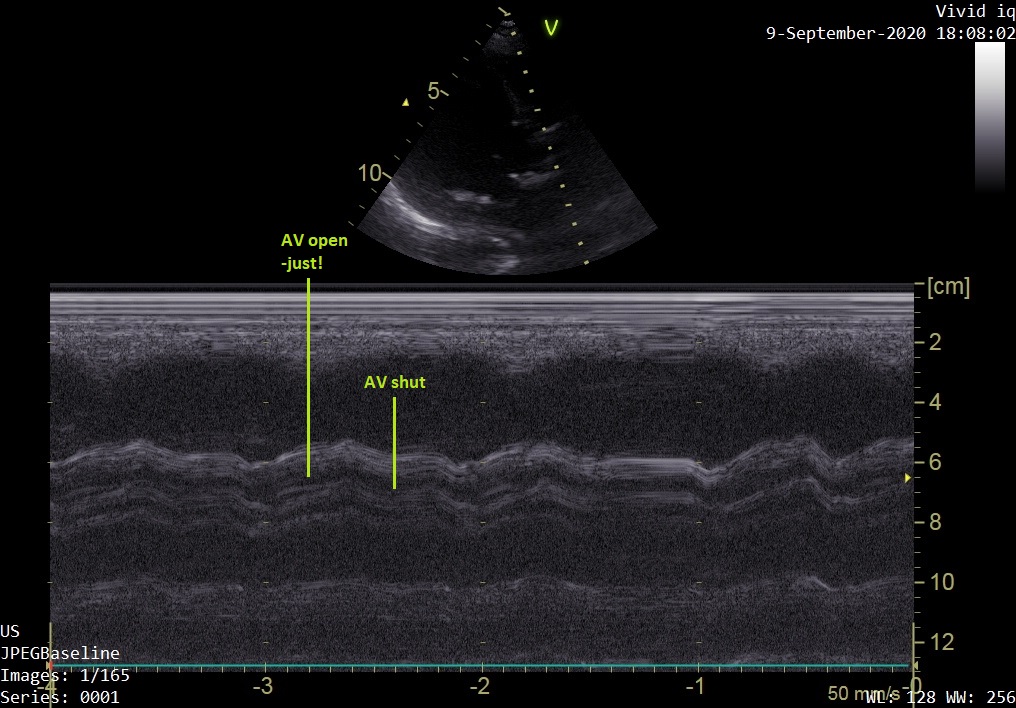
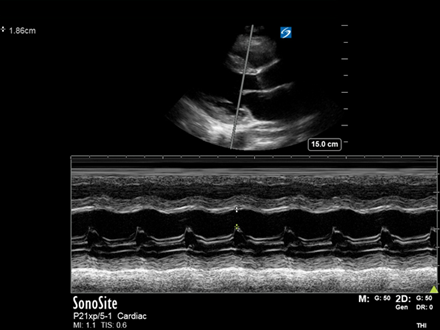
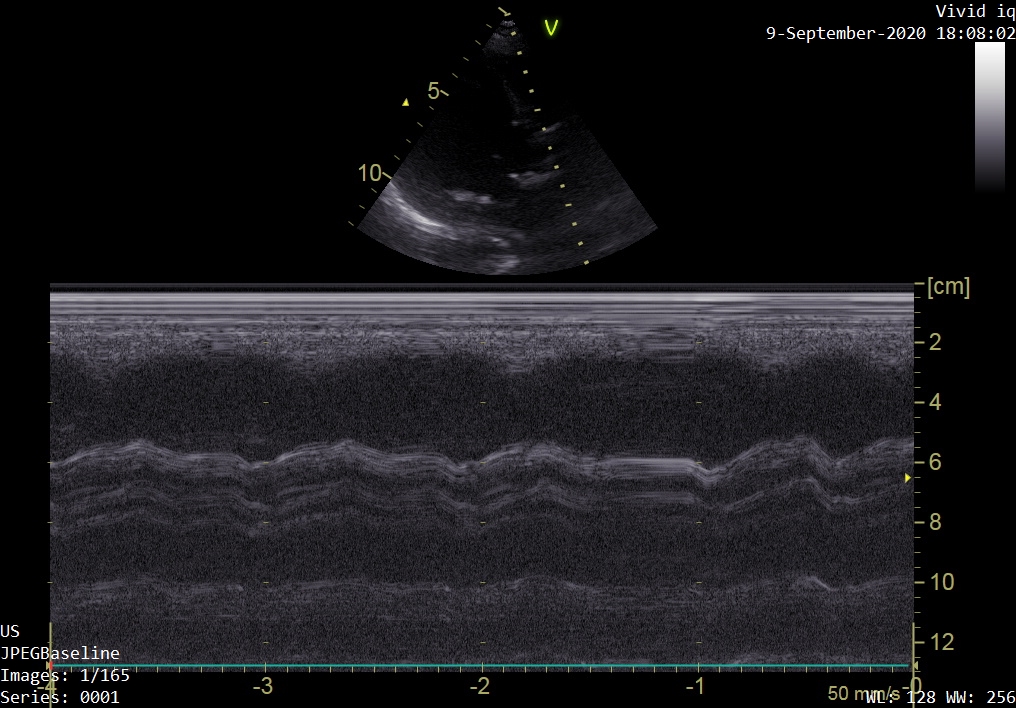
PLAX – M-mode through the AV:
Look here at the reference image of M-mode through the AV (left). Contrast this through the image of our patient (right). Our M-mode assessment of the AV confirms minimal leaflet opening.
In the A5Ch zoomed view, the AV is seen to be heavily calcified and hardly moving at all.
Conclusion:
-Hypertrophied LV with visually normal LVEF
-Normal sized RV with visually normal function
-Heavily calcified AV with very restricted opening, highly suspicious for severe Aortic Stenosis.
(N.B. a diagnosis of Aortic Stenosis cannot be made without a department comprehensive study as it requires detailed measurements. A focused study can raise suspicion though – these patients should then have a departmental echo to quantify findings.)
This patient was admitted under medics and went on to have a departmental echo confirming the above findings. He is currently under the care of cardiology for critical aortic stenosis.
[/expand]