Ultrasound of the Week #017
Case:
A man in his 60’s from a care home was brought in in severe respiratory distress, with SpO2 74% on air rising only to 92% on 15L NRBM. He was found on Chest XR to have a complete whiteout of the left lung, and consideration was given to put in a chest drain thinking this may be a unilateral pleural effusion. His ceiling of care was ward-based care, not for Optiflow/NIV and so this would be the only other intervention considered to attempt to improve his respiratory dynamics.
A lung ultrasound was performed to evaluate this further:
Question: What do these images show and what could the likely diagnoses be?
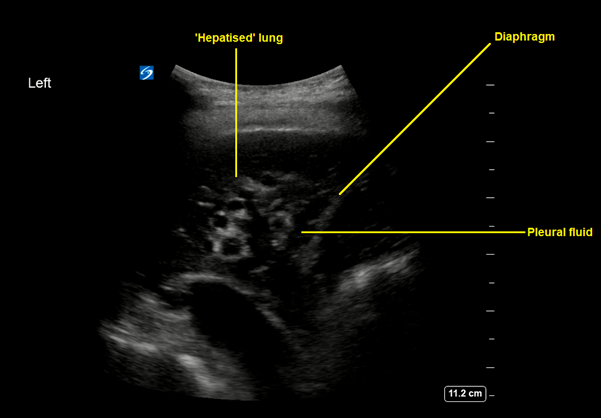
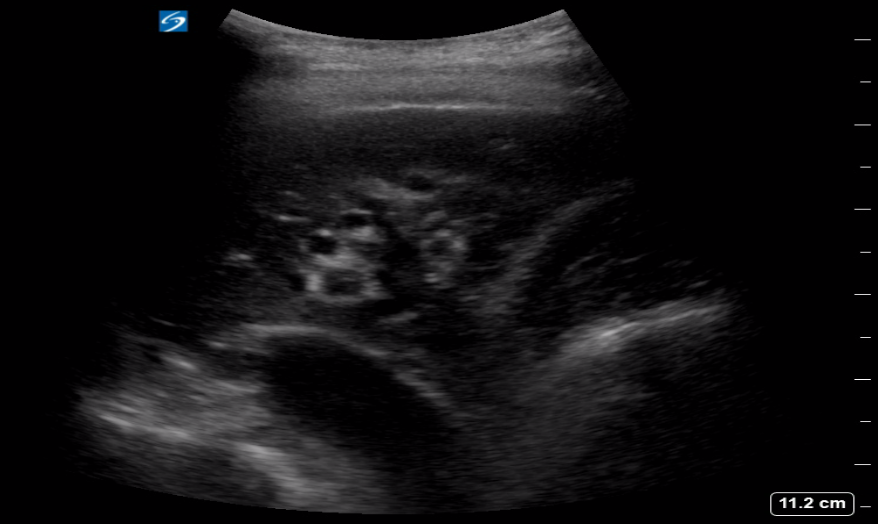
This shows dense consolidation of the left lung with a small parapneumonic effusion. The lung appearance is ‘hepatised’ and was such from top to bottom of the left lung.
Hepatisation is seen on ultrasound when lung is so densely consolidated it appears isoechoic with liver. is usually a late sign of consolidation and can also be seen in lung collapse or atelectasis. Lung ultrasound is the gold standard for imaging assessment of the pleural space and is superior to CT in evaluating pleural fluid. There is a large body of evidence for it’s high sensitivity and specificity in detecting pneumonia and indeed it is now being used a lot in the paediatric population, where it’s avoidance of ionising radiation is a great benefit.
In this case, lung ultrasound quickly identified the cause of the patient’s respiratory issues and XR changes and avoided the need for CT transfer and imaging in a very unwell patient. This patient rightly did not have a chest drain inserted and was treated with antibiotics and eventually referral to the palliative care team given his trajectory and co-morbidities.
References: